During National Nurses Week, take time to celebrate the founder of modern nursing, Florence Nightingale! Her endeavors to improve the aspect of healthcare has greatly shaped the quality of care by nurses in the 19th and 20th centuries.
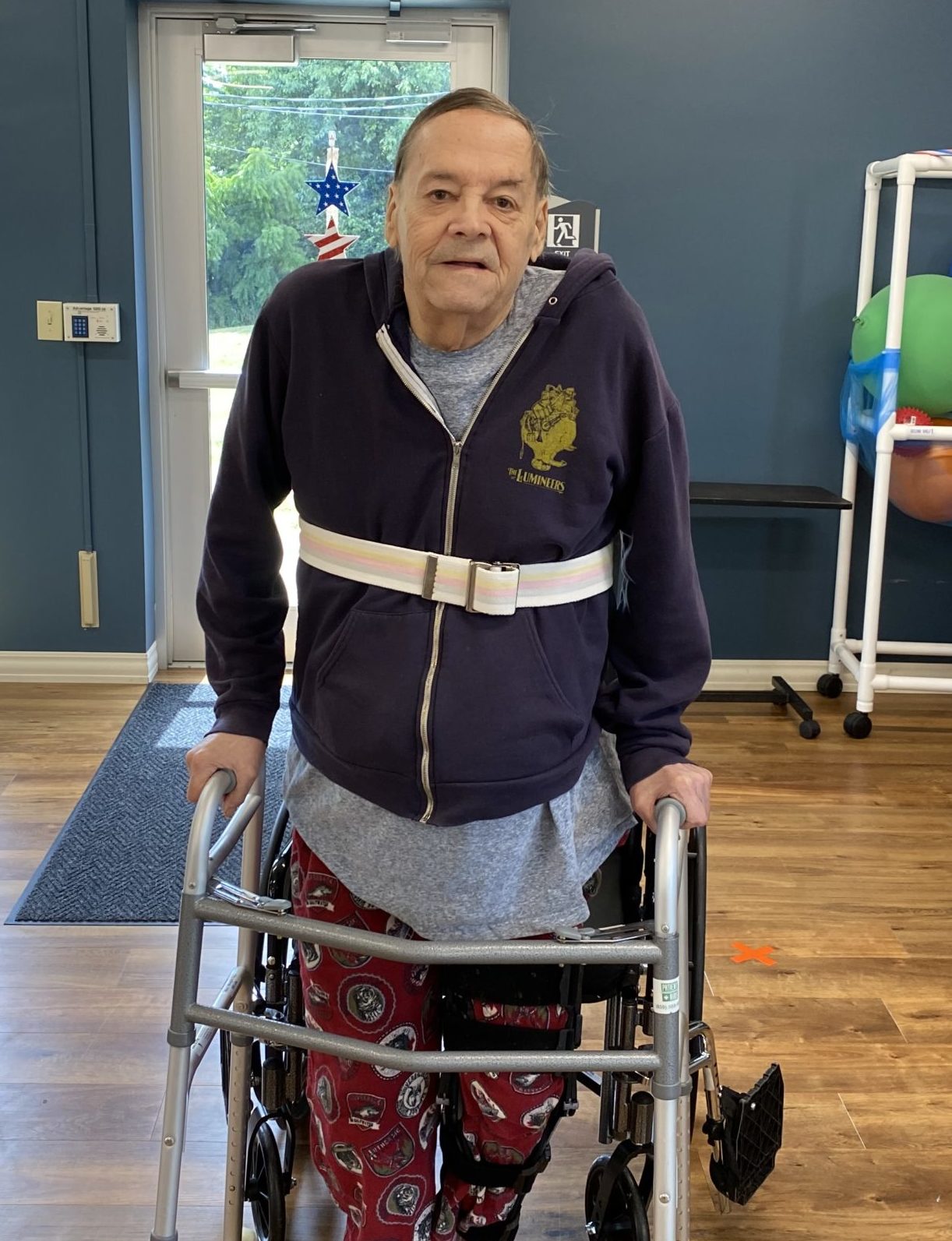
Currently, there are nurses all around the world putting their lives on the line to help stop the spread of COVID-19. It’s clear that Florence Nightingale’s impact on healthcare also helped pave the way for modern-day nurses and healthcare professionals to follow suit.
“With nurses around the world on the front lines of a global pandemic, it’s a poignant time to reflect on how Nightingale’s legacy laid the groundwork for their heroic work in hospitals today.” Says Greta Westwood, CEO of the Florence Nightingale Foundation. “She never took no for an answer – anything was possible.”
Also known as “The Lady with the Lamp”, Florence Nightingale started her nursing career in London, and later became appointed as the head nurse of the 1854 Crimean War. Nightingale’s passion and determination set her apart from others and got her the famous nickname “Lady with the Lamp” for checking on her patients via lamplight during the war. Not only did she care for her patients’ health, but she also often wrote letters to soldiers’ loved ones on their behalf.
The “Angel of the Crimea” made it her goal to lower death rates by improving hygiene practices in hospitals. She created numerous patient services that improved each patient’s quality of care while admitted in the hospital. She oversaw “invalid’s kitchen” where she set out food plans for patients that had dietary requirements. She also secured a laundry area so patients could have clean bed sheets and towels.
After the Crimean War, Nightingale wrote a book called Matters Affecting the Health, Efficiency and Hospital Administration of the British Army to share her observations and experiences while tending wounded soldiers. In 1857, the War Office’s administrative department was completely reconstruction due to Nightingale’s book and her experiences during the Crimean War, reforming several military hospitals that were under very poor conditions. (History.com Editors 2009)
In August of 1910, Nightingale became ill and was battling with heart failure. She died a week later at her home in London, bringing her life to an end at 90 years old. (History.com Editors 2009) Two years after her death, the Florence Nightingale Medal was created by the International Committee of the Red Cross, dedicated to be given to exceptional nurses every 2 years. In 1965, International Nurses Day was also created, residing on Nightingale’s birthday to continue celebrating her accomplishments. (Alexander 2018)
Despite her unexpected death, her legacy continues to live on at the Florence Nightingale Museum, which is located at the exact same spot of the original Nightingale Training School for Nurses. The museum holds over 2,000 artifacts to memorialize the mother of modern nursing. (History.com Editors 2009)
Florence Nightingale’s legacy is important to note during significant time for nurses courageously fighting on the frontlines during the pandemic. Notes Westwood, “Florence would be so proud of what nurses have managed to achieve during the pandemic.” (Haynes 2020)
References:
https://time.com/5835150/florence-nightingale-legacy-nurses/
http://history.com/topics/womens-history/florence-nightingale-1https://www.womenshistory.org/education-resources/biographies/florence-nightingale